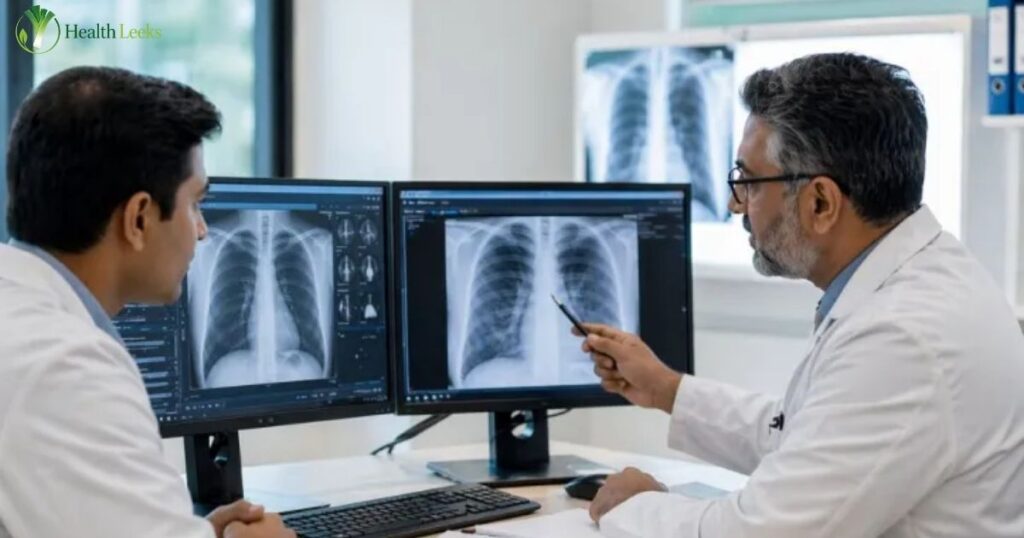
You just received your MRI, CT scan, or X-ray results, and buried in the report is a phrase that stops you cold: “Clinical correlation is recommended.” Is this a warning? A red flag? Something serious?
Take a breath. This phrase is one of the most common lines in all of radiology reporting, and understanding it can save you unnecessary worry. In this article, we break down exactly what it means, why radiologists use it, and what steps you should take next.
What Is Clinical Correlation?
Clinical correlation is a term used in medicine, frequently within radiology reports, that should be taken literally: correlate the abnormal or unexpected imaging finding with what is happening with the patient clinically.
In plain terms, it means connecting the dots. An imaging scan shows a picture of your body, but a picture alone rarely tells the full story. Clinical correlation is the process of combining:
- Your current symptoms and complaints
- Your personal and family medical history
- Findings from a physical examination
- Results from blood work or other laboratory tests
- Any previous imaging studies
Healthcare providers use the patient’s clinical findings, including medical history, physical exam, laboratory testing, and other imaging studies, to determine the true significance of radiology findings. A patient’s clinical history is essentially medicine’s Rosetta Stone for deciphering unexplained imaging results.
Why Do Radiologists Say “Clinical Correlation Is Recommended”?
Radiologists are imaging specialists. They are highly trained to read scans, but they typically work without meeting you in person or reviewing your complete medical background.
This phrase is added to a report because the doctor interpreting the X-ray or other test sees a finding that has more than one possible explanation. Since the reporting doctor is not familiar with the patient’s clinical history and examination findings, they let the patient’s treating physician make the final decision about which possibility is most likely.
Radiologists use this phrase in several specific situations:
- Inconclusive findings — Something appears unusual on the scan but may be entirely harmless, such as age-related changes in bone density or soft tissue.
- Multiple possible causes — A shadow or lesion could result from infection, inflammation, an old injury, or something more significant.
- Unexpected findings — When a radiologist sees something not expected based on the provided history, they note “clinical correlation recommended.” For example, if an abscessed tooth is seen on a CT of the face and nothing regarding this was mentioned in the history, the radiologist tells the ordering physician that something was found that they need to check out.
- Ambiguous anatomy — Certain structures look similar on imaging regardless of their underlying cause.
This is not a dismissal of your concern. It is an invitation for teamwork between the radiologist and your treating physician.
How Do Doctors Perform Clinical Correlation?
When your primary care doctor or specialist receives a report with this phrase, they begin a structured review process. This typically involves:
Step 1: Reviewing the Imaging Findings
Your doctor reads what the radiologist described, paying close attention to the size, location, and nature of any abnormality noted.
Step 2: Comparing With Your Symptoms
They then ask: Does this imaging finding explain what you are feeling? Do your symptoms match the pattern suggested by the scan?
Step 3: Checking Your Medical History
Past surgeries, medications, chronic conditions, and family history all play a role. A liver finding looks very different in a patient with a history of fatty liver disease versus a patient with no prior conditions.
Step 4: Ordering Follow-Up Tests (If Needed)
Sometimes correlation is immediate. Other times, your doctor may request additional blood tests, a follow-up scan, or a referral to a specialist to narrow down the possibilities.
The goal is to narrow down a differential diagnosis, the potential causes, to one accurate diagnosis that can account for the patient’s complete clinical picture.
The Importance of Clinical Correlation in Pathology
Clinical correlation does not apply only to radiology. It is equally critical in pathology, which is the study of tissues and cells collected through biopsies or surgical samples.
A pathologist examining tissue under a microscope may identify abnormal cells. But without knowing your age, symptoms, and medical background, even a skilled pathologist cannot always determine the final diagnosis from the slide alone.
Pathology examines tissues and cells to diagnose disease, but findings alone can be misleading. Clinical correlation, linking results to your symptoms, history, exam, and tests, is essential for accuracy and helps prevent misdiagnosis.
For example, certain inflammatory cells in a tissue sample might indicate autoimmune disease in one patient and a healing infection in another. The tissue looks the same; the context makes all the difference.
Real-Life Examples of Clinical Correlation
Understanding this phrase is easier through real-world scenarios. Here are some common examples radiologists encounter:
Example 1: Bone Lesion on X-Ray If an X-ray of the bone shows a lesion that could be produced by many different possibilities, such as a fracture, infection, or other bone pathology, the radiologist lists these possibilities. If the patient’s physician knows the patient had a prior bone fracture, that becomes the final diagnosis and the remaining possibilities are ruled out through clinical correlation.
Example 2: Brain MRI Enhancement Meningeal enhancement on a brain MRI report prompts the question: Does the patient have a known malignancy or signs of infection? The imaging finding alone cannot answer this question.
Example 3: Liver Findings Probable adenomas within the liver require clinical context: Is the patient currently taking birth control? This can cause adenomas to persist or even grow, and adenomas can bleed and cause pain.
Example 4: Gallbladder Wall Thickening Gallbladder wall thickening in a patient with ascites or liver disease could be reactive, related to third-spacing, or indicate acute cholecystitis. They can all look the same on imaging, making clinical context essential.
What Should You Do If Your Report Says This?
Reading these words on your own report can feel overwhelming. Here is a practical, step-by-step approach:
- Do not panic. This phrase appears on a large number of routine radiology reports. It is standard language, not a diagnosis.
- Schedule an appointment with your doctor. Bring the full report and any previous imaging results you have.
- Prepare your symptom history. Write down when your symptoms started, how they have changed, and anything that makes them better or worse.
- Ask questions. Ask your doctor to explain the finding, what it could mean, and what the next steps are.
- Follow through on referrals. If your doctor recommends seeing a specialist or getting additional tests, do not delay. Early clarification leads to better outcomes.
A personalized approach ensures accurate diagnosis and avoids overtreatment. Relying only on scans can lead to mistakes, while clinical correlation promotes better, patient-centered care.
Why It Matters for Your Health
Clinical correlation is not just medical procedure; it is a safeguard built into the diagnostic process to protect you.
Imaging technology is powerful, but no scan can replace the full picture of who you are as a patient. A finding that looks alarming in isolation might be entirely benign once your doctor considers your age, lifestyle, and history. Conversely, a finding that looks minor might be significant when combined with your symptoms.
Radiologists are experts at reading images, but they usually do not examine patients in person or know the full story. When they see something that could mean different things, they recommend your primary care doctor correlate it with how you are feeling and what they know about you.
This collaborative model, radiologist plus treating physician plus patient, is what makes modern medicine accurate and safe. Clinical correlation is how all three sides come together.
Frequently Asked Questions
Does “clinical correlation is recommended” mean something is seriously wrong?
Not necessarily. It is a standard phrase that simply means your doctor should review the scan result alongside your symptoms and history before drawing any conclusions.
Is this phrase the same as “correlate clinically” or “clinical correlation advised”?
Yes, these are all variations of the same recommendation and carry the same meaning in radiology and pathology reports.
Can a radiologist diagnose me without clinical correlation?
In clear-cut cases, yes. But when a finding is ambiguous or unexpected, clinical correlation is the responsible next step to avoid misdiagnosis.
Who performs the clinical correlation, the radiologist or my doctor?
Your treating physician, such as your primary care doctor or specialist, performs the clinical correlation using the radiologist’s findings as one piece of the overall diagnostic puzzle.
Should I be worried if my MRI report says this?
It is natural to feel anxious, but try not to read too much into the phrase alone. Bring your report to your doctor, who can interpret it in full context and guide your next steps.
Does clinical correlation apply only to imaging tests?
No. It also applies to biopsy results, genetic testing, blood work, and other diagnostic tests where findings need to be matched with a patient’s complete clinical picture.
Final Thoughts
The phrase “clinical correlation is recommended” is not a warning. It is a message from your radiologist to your doctor that says: there is more to this picture than imaging alone can tell. It reflects responsible, thorough medicine. Your radiologist has done their part. Now your treating physician uses that information together with everything they know about you to reach the right conclusion. If you see this phrase on your report, schedule a follow-up visit, come prepared with your symptom history, and trust the process. That is how accurate diagnosis happens.